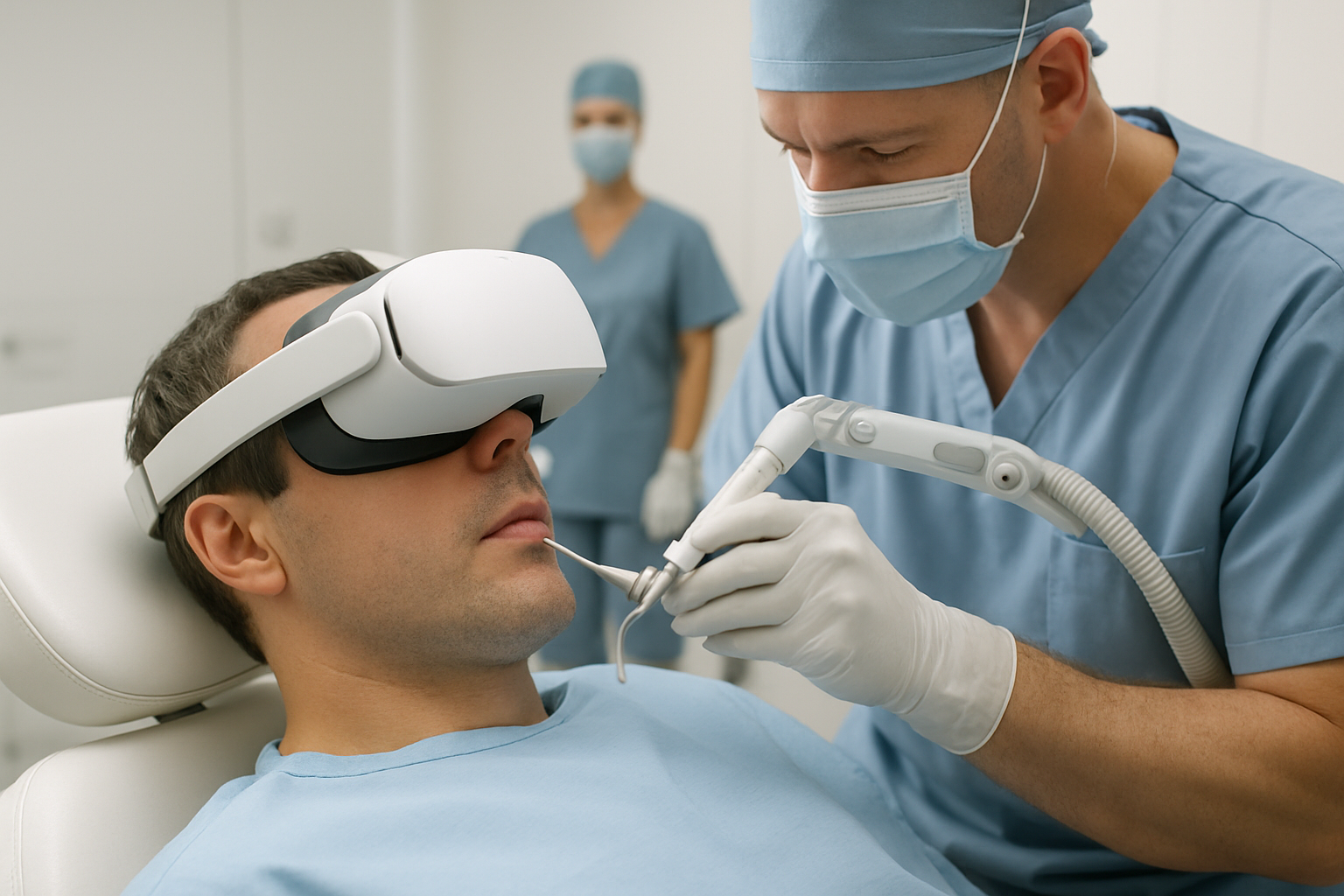
Medical professionals are revolutionizing patient care through sophisticated virtual reality protocols that induce hypnotic relaxation during surgical procedures, representing a groundbreaking advancement in healthcare technology and therapeutic innovation.
Dr. Solène Vau Quang, a pioneering stomatologist surgeon at the forefront of this technological revolution, exemplifies the new generation of clinicians integrating cutting-edge artificial intelligence and virtual reality into patient care. Her innovative approach demonstrates how advanced technology can enhance rather than replace human-centered medical practice, creating measurable improvements in patient comfort and surgical outcomes.
The Science Behind VR-Induced Hypnotic Relaxation
Virtual reality medical protocols operate by creating immersive digital environments that engage multiple sensory pathways simultaneously, effectively redirecting the patient's attention away from surgical discomfort while inducing deep physiological relaxation. The technology leverages the brain's natural capacity for neuroplasticity, using carefully designed visual, auditory, and sometimes haptic stimuli to trigger the body's relaxation response.
"During medical procedures, I use virtual reality protocols to induce a state of hypnotic relaxation. This technology provides high precision and enhanced technical capabilities while significantly improving patient comfort and clinical outcomes."
— Dr. Solène Vau Quang, Stomatologist Surgeon
The VR systems employed in medical settings differ significantly from consumer entertainment devices. Medical-grade VR equipment features enhanced hygiene protocols, precise calibration for therapeutic applications, and integration with existing hospital systems. These specialized devices can monitor patient vital signs in real-time, adjusting the virtual environment to maintain optimal relaxation levels throughout procedures.
Clinical Applications and Therapeutic Benefits
The implementation of VR hypnotic relaxation protocols spans multiple medical disciplines, with particularly notable success in oral and maxillofacial surgery, dermatology, and minor surgical procedures. Patients experience measurable reductions in anxiety, decreased pain perception, and lower requirements for pharmaceutical sedation when VR protocols are properly implemented.
Clinical studies demonstrate that VR-induced relaxation can reduce patient-reported pain levels by up to 40% during certain procedures, while simultaneously decreasing the need for traditional anesthetics and analgesics. This reduction in pharmaceutical intervention carries significant benefits, including faster recovery times, reduced side effects, and lower overall treatment costs.
Integration with Advanced Medical Technologies
The success of VR medical applications represents part of the broader "Therapeutic Revolution of 2026," characterized by prevention-first healthcare strategies and sophisticated technology integration with human-centered care approaches. This evolution parallels other major medical advances including precision medicine breakthroughs, international cooperation in healthcare innovation, and the development of minimally invasive treatment protocols.
Modern VR medical systems integrate seamlessly with existing diagnostic and surgical equipment, providing real-time biometric monitoring while maintaining the immersive therapeutic experience. Advanced algorithms adjust virtual environments based on patient responses, ensuring optimal therapeutic efficacy while maintaining safety protocols essential for medical applications.
Global Adoption and Healthcare Transformation
The adoption of VR medical protocols aligns with international trends toward prevention-focused healthcare strategies that emphasize patient comfort and improved outcomes over purely reactive treatment models. Countries implementing comprehensive technology integration programs report enhanced community resilience, reduced emergency care demands, and measurable improvements in patient satisfaction metrics.
Healthcare systems worldwide recognize VR medical applications as cost-effective alternatives to traditional sedation methods, particularly valuable in resource-constrained environments where pharmaceutical options may be limited. The technology's portability and reusability make it especially attractive for developing healthcare infrastructure and mobile medical units.
Training and Implementation Challenges
Successful VR medical implementation requires comprehensive professional training programs ensuring healthcare providers understand both technological capabilities and therapeutic applications. Medical schools increasingly incorporate VR training modules into curricula, preparing future practitioners for technology-enhanced patient care delivery.
Implementation challenges include equipment costs, staff training requirements, and integration with existing hospital information systems. However, economic analyses demonstrate that initial technology investments are justified through long-term savings in pharmaceutical costs, reduced procedure times, and improved patient outcomes leading to decreased complications and readmissions.
Future Developments and Research Directions
Current research explores expanding VR medical applications beyond procedural relaxation to include therapeutic interventions for chronic pain management, post-traumatic stress disorder treatment, and rehabilitation programs. Scientists investigate combining VR protocols with other emerging technologies including artificial intelligence diagnostics, precision medicine approaches, and personalized therapeutic interventions.
International cooperation drives continued innovation through peer-to-peer knowledge sharing networks, bilateral partnerships, and coordinated research initiatives. This collaborative approach ensures VR medical advances benefit diverse populations regardless of geographic or economic constraints, supporting the global transition toward more accessible, effective healthcare delivery systems.
Patient Safety and Regulatory Considerations
Medical VR systems undergo rigorous safety testing and regulatory approval processes ensuring patient welfare remains paramount throughout technological integration. Regulatory frameworks address concerns including device sterilization, electromagnetic interference with medical equipment, and protocols for patients with specific medical conditions that might contraindicate VR use.
Healthcare institutions implementing VR protocols develop comprehensive safety guidelines covering equipment maintenance, staff certification, patient screening, and emergency procedures. These protocols ensure that technological innovation enhances rather than compromises patient safety while maintaining the high standards expected in medical environments.
Economic Impact and Healthcare Sustainability
VR medical applications contribute to sustainable healthcare delivery through multiple economic mechanisms. Reduced pharmaceutical consumption, shorter procedure times, improved patient satisfaction, and decreased complication rates create measurable cost savings that justify technology investments while improving overall care quality.
The technology's potential for medical tourism development and international healthcare cooperation creates additional economic opportunities. Healthcare systems investing in advanced VR capabilities position themselves as regional medical destinations, attracting patients seeking innovative treatment options while building expertise that benefits local populations.
Looking Ahead: The Future of VR Medicine
March 2026 represents a critical juncture in healthcare evolution, with VR medical applications demonstrating how technological innovation can address 21st-century health challenges through coordinated international action and sustained commitment to patient-centered care. The convergence of precision medicine advances, international cooperation models, and prevention-focused strategies provides a robust foundation for resilient healthcare systems.
As VR medical protocols continue evolving, their integration with artificial intelligence, personalized medicine approaches, and global healthcare networks promises even greater therapeutic possibilities. Success depends on maintaining the balance between technological advancement and human-centered care principles, ensuring that innovation serves to enhance rather than replace the fundamental doctor-patient relationship that remains at the heart of effective medical practice.